New studies shine light on need for long COVID research in PH
MANILA, Philippines—In May this year, it was announced that the government has begun focusing on “long COVID cases.” However, since then, little to no update has been made available to the public.
According to World Health Organization (WHO), long COVID, also known as “post-COVID condition,” refers collectively to various long-term symptoms that some people experience after they have had COVID-19.
The condition is also called long COVID, long-haul COVID, post-acute COVID-19, post-acute sequel of SARS CoV-2 infection (PASC), long-term effects of COVID, and chronic COVID by others.
People who experience it refer to themselves as “long-haulers.”
“Post COVID-19 condition is defined as the illness that occurs in people who have a history of probable or confirmed SARS-CoV-2 infection., usually within three months from the onset of COVID-19, with symptoms and effects that last for at least two months,” WHO explained.
Article continues after this advertisementOn May 22, Dr. Ted Herbosa, an adviser to the National Task Force against COVID-19, said that medical professionals “are starting to see cases of long COVID” in the Philippines. He added that the government has started focusing on the condition.
Article continues after this advertisement“We are monitoring and recording it. We will also register it and we will count and study it so that we will know the situation of long COVID in the Philippines,” he said.
It was the first time health authorities confirmed long COVID among Filipinos.
READ: Gov’t now also focusing on ‘long COVID’ cases
However, little to no update regarding long COVID cases in the country has been officially announced or made available to the public since then.
In this article, INQUIRER.net will detail recent findings from several studies across the globe, emphasizing the reasons that studies and discussions on long COVID cases in the Philippines are crucial.
What we know so far
Prior to Herbosa’s statement, in January, Health Undersecretary Leopoldo Vega has already warned that 10 percent to 15 percent of COVID-19 patients might be afflicted with long COVID.
Vega explained that if a person who recently recovered from COVID-19 continues to experience health issues after 30 days, chances are he or she has long COVID.
According to WHO, anyone who has had COVID-19 can develop long COVID and experience prolonged symptoms. The US Centers for Disease Control and Prevention (CDC) noted that certain groups of people are likely to be affected more by long COVID based on previous studies.
These include people who have experienced more severe COVID-19 illness, had underlying health conditions prior to COVID-19, those who did not get a COVID-19 vaccine, and individuals who experience multi-system inflammatory syndrome (MIS) during or after COVID-19 illness, among others.
WHO also found that 30 percent of people experience long COVID six months after hospitalization due to COVID-19, 13.3 percent experience long COVID a month or more after initial infection, and 2.5 percent experience long COVID three months or more after contracting COVID-19.
Since there is not enough data yet on long COVID, health experts said it is still difficult to predict how long the post-COVID-19 condition will last for a patient.
“There is much to learn about the post-COVID-19 condition, but current research shows that patients can experience lingering symptoms for weeks to months following COVID-19. The research also shows that patients can improve with time,” WHO said.
An article on the American Medical Association’s (AMA) website titled “What doctors wish patients knew about long COVID,” noted that there are three types or categories of long COVID, including:
- first category: people with COVID who don’t recover completely and have lasting symptoms because of cell damage
- second category: people with COVID who had been in ICU and in bed for weeks
- third category: people with COVID symptoms appearing after recovery.
Among the commonly reported symptom of long COVID were general symptoms such as tiredness, fever, and others that get worse after physical or mental effort (post-exertional malaise).
Various respiratory and heart symptoms, neurological symptoms, and digestive symptoms have also been reported by some.
However, the US CDC and the Department of Health (DOH) emphasized that not all long haulers experience the same symptoms.
“Post-COVID conditions may not affect everyone the same way. People with post-COVID conditions may experience health problems from different types and combinations of symptoms happening over different lengths of time. Most patients’ symptoms slowly improve with time,” the US CDC said.
In a statement released last May 22, the DOH also advised Filipinos to consult a doctor or health care provider if they experience prolonged COVID-19 symptoms or symptoms related to long COVID.
READ: Understanding ‘long COVID’ and how to prevent it
More data, better insight
In the United States, several studies have been done and published in the past months about long COVID. Recent data collected by the US Census Bureau and the US CDC provided a closer look at long COVID cases among Americans.
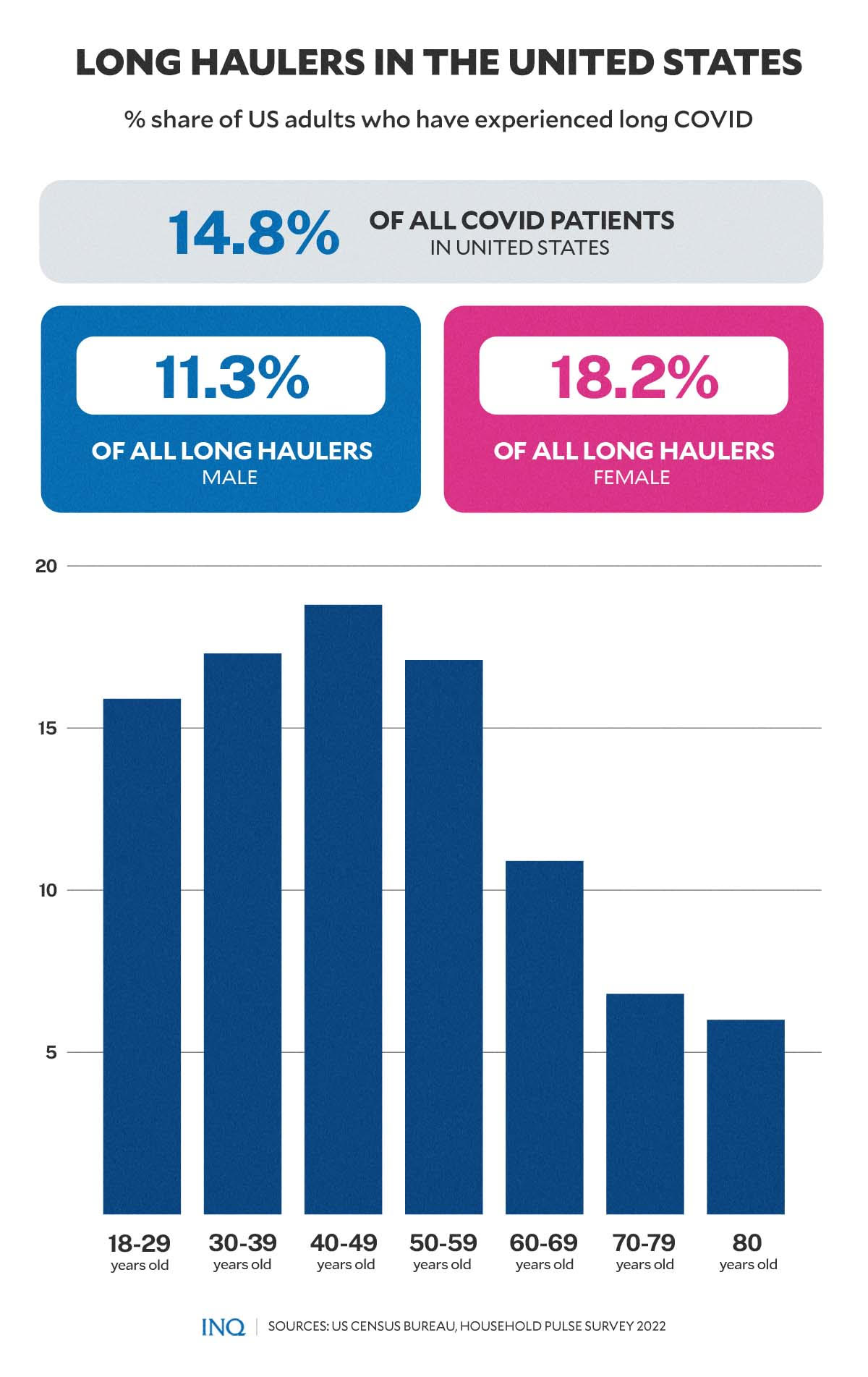
Based on the Census Bureau’s Household Pulse Survey (HPS), 14.8 percent of 46,190 US adults surveyed between July 27 to August 8 have “ever experienced post-COVID conditions (long COVID).”
These adults had COVID and had some symptoms that lasted three months or longer,” the US CDC said.
The HPS survey asked respondents four questions:
- “Have you ever tested positive for COVID-19 (using a rapid point-of-care test, self-test, or laboratory test) or been told by a doctor or other health care provider that you have or had COVID-19?”
- “How would you describe your coronavirus symptoms when they were at their worst?”
- “Did you have any symptoms lasting 3 months or longer that you did not have prior to having coronavirus or COVID-19?”
- “Do you have symptoms now?”
The survey further found that more female respondents have had at some point—or currently have—long COVID (18.2 percent) compared to male respondents (11.3 percent).
It also detailed the portion of US adults who currently have experienced—or currently have—long COVID depending on their age groups:
- 18-29 years: 15.9
- 30-39 years: 17.3
- 40-49 years: 18.8
- 50-59 years: 17.1
- 60-69 years: 10.9
- 70-79 years: 6.8
- 80 years: 6.0
Long haulers in labor sector
Aside from gathering data that could provide better insight on long COVID cases and situations in the country, studies on the condition also give a better idea of how COVID-19—specifically post-COVID condition—impacts the labor sector.
According to US Census Bureau’s estimates based on June to July HPS survey, there are currently 16.3 million individuals—around 8 percent of working-age Americans—who currently experience long COVID.
Several other research gave estimates on how many working-age Americans have had long COVID.
A study published last July 7 by the Federal Reserve Bank of Minneapolis found that 24.1 percent of US adults who have contracted COVID-19 experienced symptoms that lasted for over three months—which, the author said, could be considered long COVID.
Data from the US CDC showed that around 70 percent of Americans have contracted COVID-19.
“If 24.1% of them (70 percent of Americans who contracted COVID-19) have had long COVID, 34 million working-age Americans have, at some point, had long COVID,” a report published by the Brookings Institution—a Washington-based nonprofit public policy organization—noted.
“The Minneapolis Fed study found that 50% of respondents had recovered from long COVID. If we exclude that 50%, we are left with around 17 million people who may currently have long COVID—very near the HPS estimate of 16.3 million,” the report added.
Out of work due to long COVID
Long COVID, according to research, impacts work and causes affected individuals to leave the workforce or reduce their working hours due to persistent symptoms.
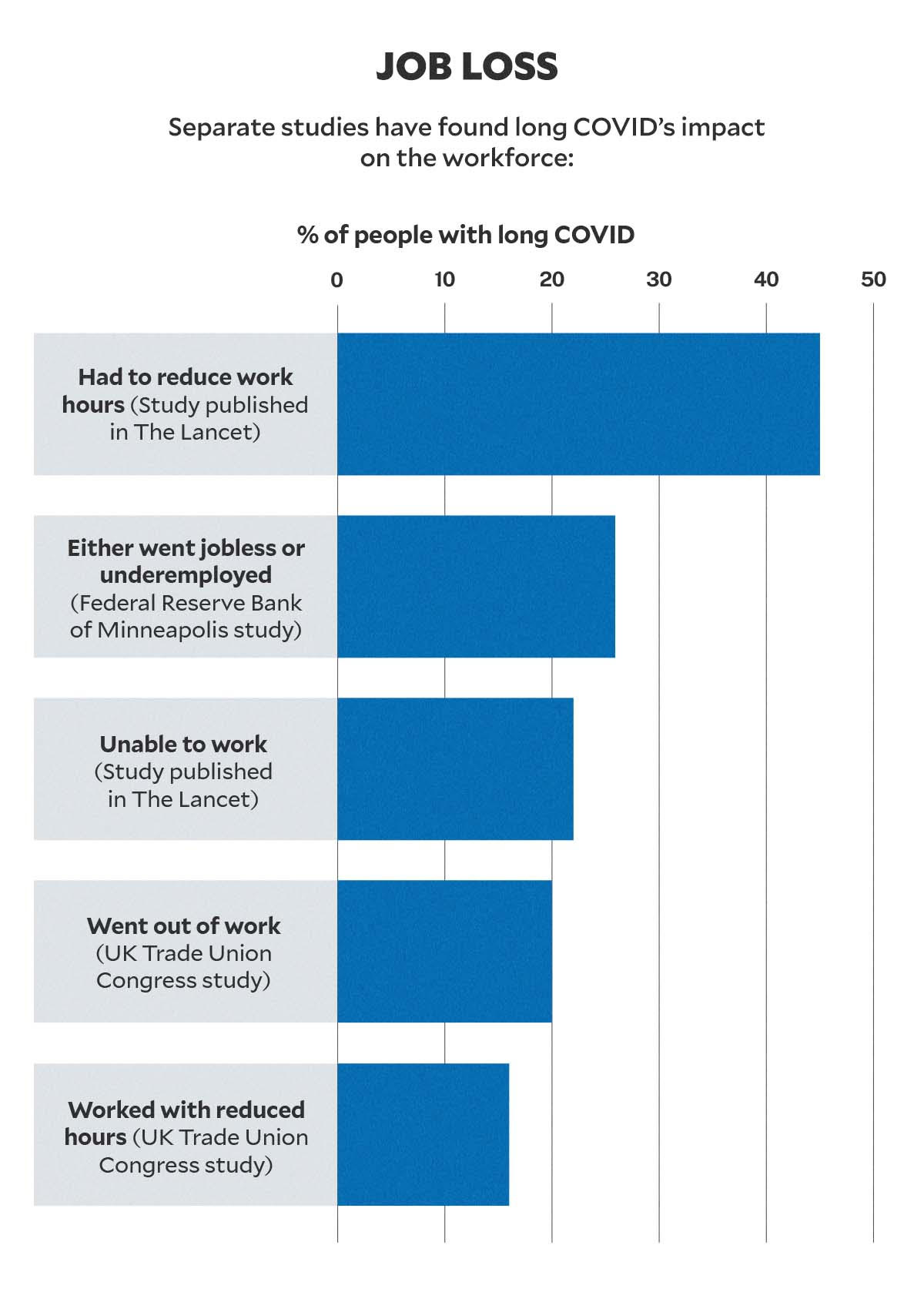
The same study by the Federal Reserve Bank of Minneapolis found that 25.9 percent of people with long COVID have had their work “impacted”—“meaning that they are either out of work or working reduced hours.”
A separate study published in The Lancet discovered that 22 percent of people with long COVID were not able to work due to ill health, while another 45 percent had to reduce their work hours—both groups cited cognitive dysfunction or memory issues due to post-COVID conditions.
In the United Kingdom, a survey from the Trades Union Congress (TUC) found that 20 percent of people with long COVID were not working, and 16 percent more were working reduced hours.
According to WHO, long COVID could cause symptoms that can disrupt a person’s ability to perform daily tasks, including work.
“While most people who develop COVID-19 fully recover, long haulers develop a variety of mid-and long-term symptoms such as fatigue, breathlessness, and cognitive dysfunction (for example, confusion, forgetfulness, or a lack of mental focus and clarity). Some also experience psychological effects as part of the condition,” said WHO.
“These symptoms might persist from their initial illness or develop after recovery. They can come and go or relapse over time—which, as a result, affects a person’s ability to perform daily activities such as work, studies, or household chores,” WHO added.
New findings: Impact on brain
In May, a study published in Nature Medicine titled “Long COVID after breakthrough SARS-CoV-2 infection” detailed that “post-acute sequelae of COVID-19”—in simple terms, long COVID—could increase the likelihood or risk of having new health conditions, including:
- Cardiovascular: 2.36 percent
- Coagulation and hematologic: 2.22 percent
- Diabetes: 1.62 percent
- Fatigue: 2.4 percent
- Gastrointestinal: 1.69 percent
- Kidney: 1.7 percent
- Mental health: 1.97 percent
- Musculoskeletal: 1.29 percent
- Neurologic: 1.39 percent
- Pulmonary: 2.49 percent
READ: COVID can reinfect you, raise health risks: What to know
A study published in The Lancet last August 17 found that long COVID impacts the brain and causes the following:
- overall reduction in the size of the brain
- mental health complaints and neurological defects (depression, anxiety, mood disorders, and cognitive impairment)
- dementia-like problems (brain fog, memory loss)
- psychosis
- seizures
The study noted that in long COVID anxiety and mood disorders “tend to resolve over months,” while serious dementia-related problems, psychosis, and seizures persist for at least a couple of years.