Mammograms should start at 40, says US task force
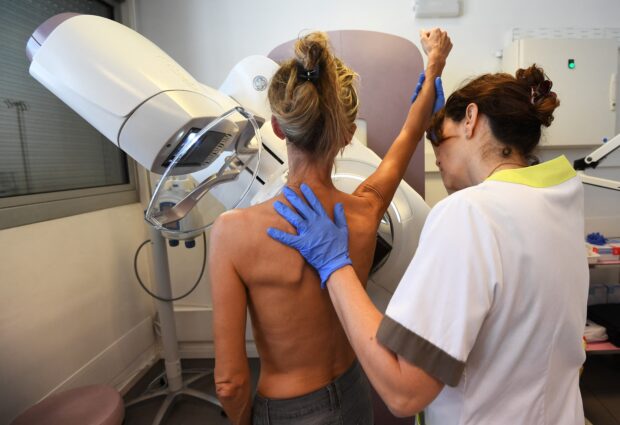
In this file photo taken on October 09, 2017, a patient is pictured before a mammography at the Paoli-Calmette institute, a fight against cancer regional center. AFP
WASHINGTON — All women should get mammogram screening for breast cancer starting from age 40, rather than 50, an influential US health body announced Tuesday, a move it said could save thousands of lives.
Breast cancer is the second most common cancer and the second most common cause of cancer death for women in the United States, killing around 42,000 women and 500 men, according to official data. Black women are 40 percent more likely to die than white women.
The Preventive Services Task Force, a group of independent experts appointed by the Department of Health and Human Services, said that while it previously recommended women in their 40s make individual choices about when to start screening, the new guidance could result in 19 percent more lives being saved.
“New and more inclusive science about breast cancer in people younger than 50 has enabled us to expand our prior recommendation and encourage all women to get screened every other year starting at age 40,” said the Task Force in a statement.
Based on the evidence, the new recommendation was assigned a “Grade B” rating, its second highest level.
Article continues after this advertisementThe guidance is still considered a draft, with the Task Force posting the evidence it considered on its website and allowing time for public comments and review. American health insurance is required to cover any service USPSTF recommends, regardless of cost.
Article continues after this advertisement“Ensuring Black women start screening at age 40 is an important first step, yet it is not enough to improve the health inequities we face related to breast cancer,” added Task Force vice chair Wanda Nicholson.
“In our draft recommendation, we underscore the importance of equitable followup after screening and timely and effective treatment of breast cancer and are urgently calling for more research on how to improve the health of Black women.”
The draft recommendation applies to women at “average risk” of breast cancer, which includes people with a family history of breast cancer or other risk factors such as having dense breasts, which about half of all women do.
It doesn’t apply to people who have a prior history of breast cancer, or who have certain genetic markers that place them at high risk, have had high-dose radiation therapy from a young age, or had high risk lesions taken on biopsies.
The body said there was lingering uncertainty when it came to the benefits and harms of screening people aged 75 and older.
“The balance of benefits and harms may shift as women age, but there is very limited research on this age population,” it said in a statement.
The Task Force said more research was needed to determine whether women with dense breasts should have additional screening with ultrasound or MRI, since mammograms may not work as well for them.
Annual screening?
Sarah Friedewald, chief of breast imaging at Northwestern Medicine, told AFP that while she applauded the Task Force for recognizing age 50 was too late to start screening, “We feel very strongly that it should be every year.”
“If you increase the interval between the screens, you just allow the cancers to grow larger and potentially less treatable,” she said, adding her recommendation was backed by numerous clinical trials and modeling data.
When tumors are caught early, they can be surgically removed, without resorting to breast removal.
The main risks linked to mammograms, X-ray pictures of the chest, are anxieties associated with patients getting called back for additional imaging and biopsies that often turn out to be benign. The radiation risk associated with mammography is minimal.
RELATED STORIES