‘Suicide mission’: Cutting short isolation of health workers with COVID
MANILA, Philippines — The rationale for a government proposal to shorten isolation periods for health workers infected by the COVID virus has been explained as an answer to manpower shortages but a group of nurses likened it to sending health professionals on a “suicide mission.”
It’s clear, though, that the resolution issued by the Inter-Agency Task Force on Emerging Infectious Diseases (IATF) to cut short the period of COVID-related absences of health workers is drawing controversy and concern among those on the frontline of the health crisis.
READ: IATF finds way to avert hospital staff shortage
On Jan. 6, Cabinet Secretary Karlo Nograles, also acting Palace spokesperson, said the IATF has approved a resolution allowing health care workers infected with coronavirus to return to work after an isolation period that was cut by half—from 10 to five days.
A nurses’ group, Filipino Nurses United (FNU), questioned the resolution, saying it mirrored the government’s “chaotic response” to the COVID crisis. “That is not safe, not fair and irrational,” the group said in a statement.
FNU, which advocates for nurses’ rights and welfare, said the reduced period for infected health care workers’ isolation “will compromise our health and safety” and put patients and communities at greater risks.
Article continues after this advertisementJaymee de Guzman, who works at the San Lazaro Hospital, told INQUIRER.net that with the shortened isolation period, “we will literally become the spreaders of the virus.”
Article continues after this advertisementShe said health care workers already suffered discrimination in 2020, when the pandemic reached Philippine shores, even as they tested negative for coronavirus. “How much more now?” De Guzman said.
‘Preventing dry out’
Nograles said during President Rodrigo Duterte’s Talk to the People that the shortened period of quarantine for health care workers was a way to prevent hospitals from suffering a shortage of professionals who would take care of COVID patients.
The IATF’s Resolution No. 156 came as COVID-19 cases hit record highs and over 700 health care workers fell ill. This gave rise to the suspension of out-patient and emergency services in some hospitals.
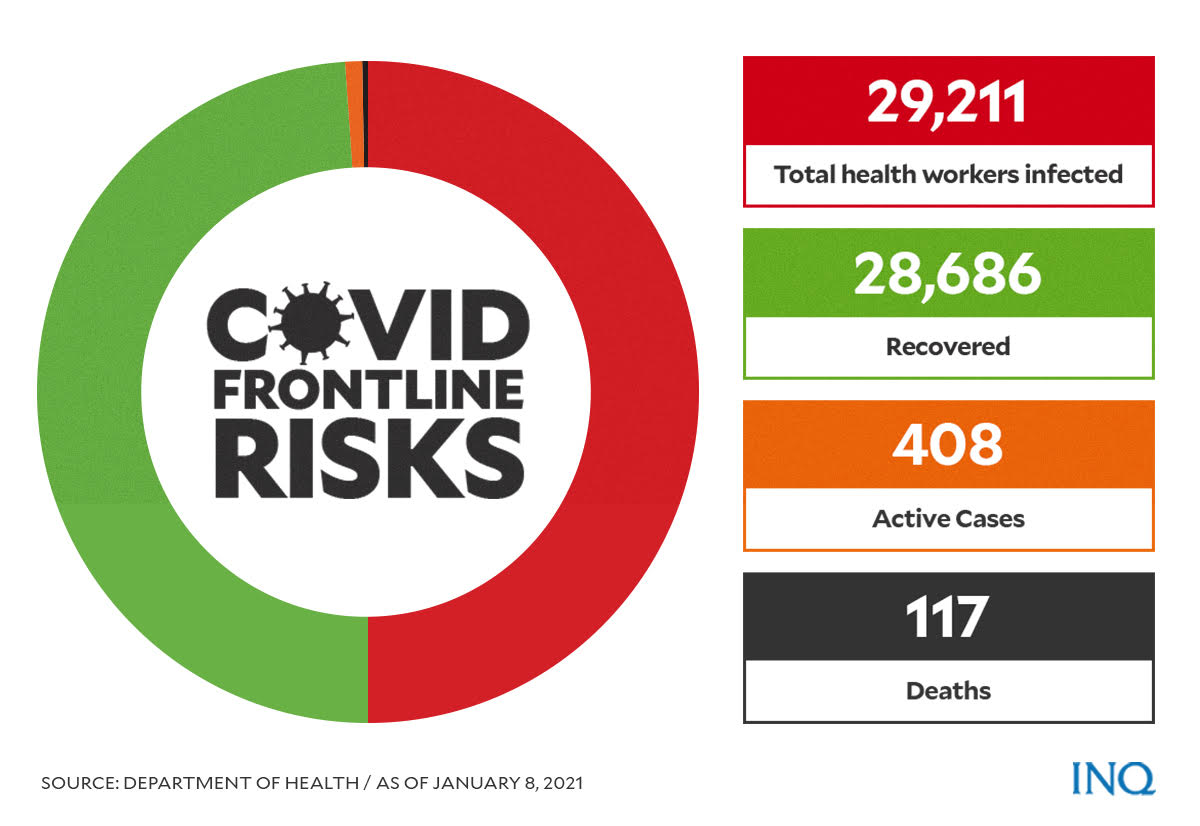
The Department of Health (DOH) said on Jan. 10 that since March 2020, there were 29,609 health care workers infected by coronavirus: 28,723 have recovered, 117 have died, while 769 are still sick.
Among health workers, who are still sick, at least 581 (75.6 percent) have mild cases, 167 (21.7 percent) don’t have symptoms, 10 (1.3 percent) have moderate cases, nine (1.2 percent) have severe cases and two (0.3 percent) are in critical condition.
On Jan. 5, the Philippine General Hospital (PGH), which is in “crisis mode” because 310 of its 2,000 health care workers contracted COVID, said its emergency room would accept only these cases—stroke, accidents, heart attacks and other life-threatening emergency cases.
The out-patient department of the Tondo Medical Center, Dr. Jose Fabella Memorial Medical Hospital and the Philippine Orthopedic Center have been temporarily closed. The Gat Andres Bonifacio Medical Center closed its emergency room.
De Guzman said while nurses expected a rise in COVID-19 cases because of Omicron, a variant of Sars COV2, and eased restrictions, they were overwhelmed by the increase in symptomatic patients arriving at the San Lazaro Hospital to seek medical help.
A nurse at the COVID-19 triage area where the sick are being assessed for RT-PCR tests, De Guzman said nurses in the hospital used to attend to 100 to 150 individuals daily before the new COVID surge. “We are now having 350 every day and there was even a time when we had 500,” she said of the new average daily number of patients.
She said that San Lazaro Hospital currently has 127 COVID-positive health care workers: 66 are nurses, 44 are medical staffers, 14 are administrative staffers and three are casual employees. “We have no extraordinary protection from the virus. We’re only like other people,” she said.
“We’re already exhausted. Since a lot of workers here have tested positive for COVID and we are already on a skeletal work arrangement, things became really difficult, especially with the increase in patients. It’s really tiring,” she said.
No rest from battle
Nograles said the new directive allows hospitals to cut short to five days the quarantine period for fully vaccinated health workers who are exposed to COVID patients.
He said that in “extreme circumstances,” while weighing the risks and benefits, the isolation protocols could be adjusted to a shorter period for fully vaccinated health care workers who are themselves sick with COVID.
Nograles explained that quarantine and isolation are different things–the first is for individuals who are exposed to COVID patients while isolation is for mild cases and COVID patients who don’t have symptoms.
On Jan. 7, Health Undersecretary Maria Rosario Vergeire said hospitals would be allowed to require only a five-day isolation period for health care workers who don’t have symptoms or have mild to moderate COVID cases.
Isolation, which was reduced to five days, usually takes 10 days, while quarantine, which usually takes seven days, may now be waived by fully vaccinated health care workers, Vergeire said.
She, however, explained that hospitals and provincial health offices would have to thoroughly study the situation before enforcing the new IATF resolution and this would depend highly on hospital conditions.
De Guzman said while the directive could be based on what is “practical”, it appeared that health care workers had become “sacrificial lambs.”
“Right now, the period was shortened since they need health care workers because without us, the health care system could collapse,” she said.
‘Things will get worse’
Eleanor Nolasco, FNU vice president, told INQUIRER.net that the latest IATF directive “could make things even worse” because hospital settings are where there’s an increased chance of infection and exposure to COVID patients.
“The period they are giving is not enough for health care workers to completely recover,” she said, explaining that while nurses still commit themselves to fighting the COVID crisis, they will not agree to a “suicidal” mission.
De Guzman said COVID is often associated with physical weakness and health care workers are not exempt from this. “How will you work well? Your body is weaker compared to when you’re not infected with the virus,” she said.
Nolasco said the health care system, which is “chaotic and not prepared” for the COVID crisis, could even get worse with a directive which outrightly disregards health care workers’ safety and welfare.
“We are already placed at greater risk of contracting the disease,” Nolasco said, listing the exponential rise in the number of COVID patients, extended work hours and “chronic” manpower shortages as some of the biggest challenges that health professionals face.
‘Gamble’
The US Center for Disease Control and Prevention (CDC) said health care workers in the United States who have no symptoms may return to work after seven days of isolation, provided they test negative at the end of the isolation period. A 10-day isolation had been previously recommended.
This, however, was condemned by the National Nurses United group in the US which asked the CDC last Dec. 29 to reverse its decision. It said the reduced isolation period will only result in increased transmission, illness and death.
Dr. Amir Khan, a health expert, said in Al Jazeera’s Doctor’s Note that the World Health Organization WHO continues to recommend isolation of 14 days for people who test positive for coronavirus. At least two countries—Germany and Jordan—continue to heed this, he said.
He said a study that was published in JAMA Internal Medicine last year found that people with COVID-19 were “most infectious two days before and three days after they develop symptoms.”
The problem, however, is that the data only refers to some, not all, people and that COVID-19 is unpredictable, he said, explaining that reducing the isolation period is like a “gamble”.
‘Gov’t not mindful’
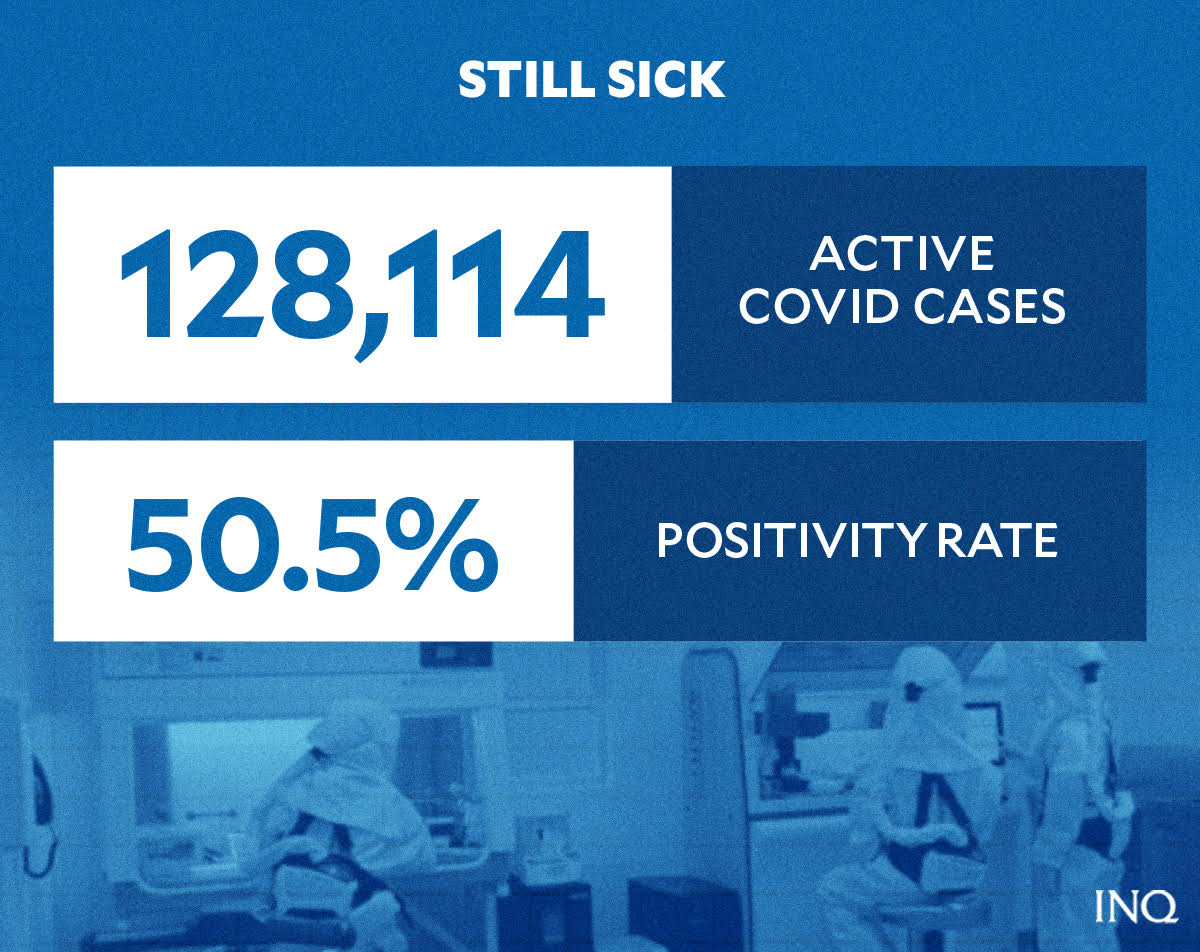
The DOH, on Jan. 10, said the Philippines has 157,526 active cases because of a record 33,169 new COVID-19 cases. The positivity rate–the percentage of people who test positive out of total tests at a certain period–was 46.0 percent with 73,234 individuals tested.
READ: PH records 33,169 new COVID-19 cases amid Omicron scare
Currently, 38 percent of intensive care unit (ICU) beds, 41 percent of isolation beds, 41 percent of ward beds and 17 percent of ventilators in the Philippines are in use.
In Metro Manila, 52 percent of ICU beds, 54 percent of isolation beds, 67 percent of ward beds and 25 percent of ventilators are in use mainly because of a surge in cases being attributed to Omicron, a coronavirus variant said to be more contagious.
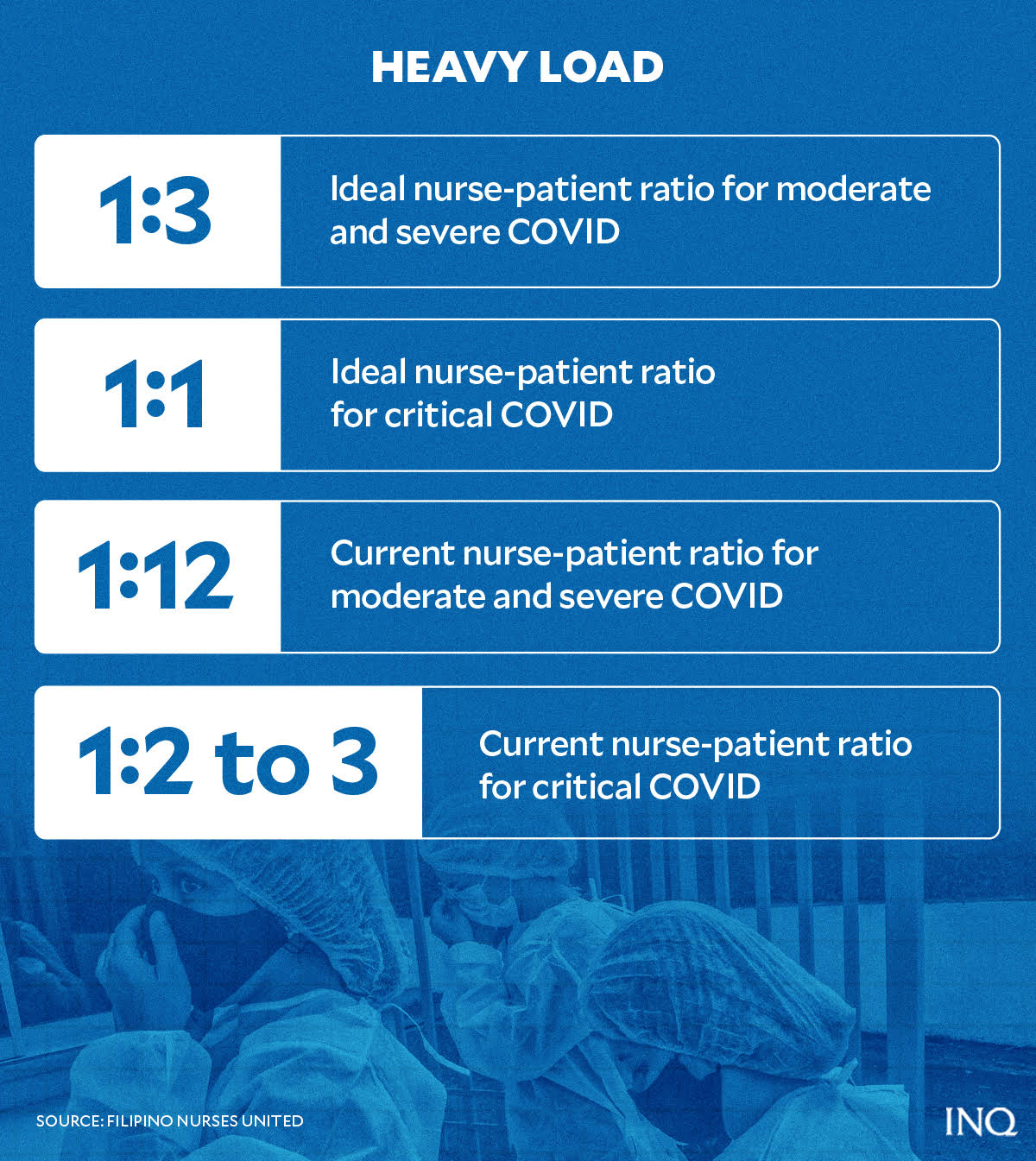
FNU previously said the ideal nurse-to-patient ratio in COVID wards is 1:3 for moderate to severe cases and 1:1 for critical cases. But currently, one nurse handles as many as 12 patients with severe COVID and two to three patients in ICU.
Nolasco said even before the COVID crisis hit, hospitals were already experiencing lack of health care workers. “There’s a lot of individuals who are resigning or are transferring to other kinds of work.”
READ: Nurses’ exodus: Hailed as heroes, treated like peons
“There’s a heavy pressure and it’s really hard to work in a hospital because the government wasn’t able to fill the gaps in the chronic lack of health care workers in the Philippines,” she said.
She said the new IATF directive has “demoralized and disincentivized” health workers. “That’s one of the reasons why we oppose,” she explained, saying the added risks piled up on top of lack of benefits and lack of security of tenure for nurses.
READ: Health care workers’ benefits: ‘Singular’ plan brings multiple issues
The Department of Labor and Employment had estimated the compensation levels of nurses in the Philippines:
- Entry-level registered nurse — P8,000 to P13,500 per month
- Registered nurses hired but not regular at private hospitals—average salary of P9,757 per month
- Average salary in government hospitals — P13,500 per month
- Average salary in private sector — around P10,000 per month
Test, hire
Nograles said if health care workers should not be kept away from COVID duty for a lengthy period because “we don’t want us to dry out of health care workers who would man our hospitals.” This was the reason for IATF Resolution No. 156, he said.
Nolasco, however, said reducing the isolation period for health care workers will not solve the problem of manpower shortage. “The government should get resources and test health care workers,” she said.
She explained that the government should be reminded that it has a responsibility to protect health care workers by providing safe work environments with reduced risks of coronavirus infections.
She said DOH data revealed that nurses, which comprise 70 percent of the health care workforce in the Philippines, are still the most at-risk with over 10,000 nurses, or 70 percent of total, being infected with coronavirus.
Nolasco asked the government to not only provide additional beds in health facilities. She said the government should hire more health care workers to fill the “chronic gap” in personnel needed for critical health care services.
FNU said the government should hire the needed 50,000 nurses for 42,000 barangays and public hospitals in the Philippines. “They should be in regular or permanent positions to resolve the issue of understaffing and patient safety.”
“The public health measures for infection control should be strongly improved with free and accessible COVID-19 tests, aggressive and systematic contact-tracing and improved quarantine services, alongside adequate aid and socio-economic assistance for displaced sectors,” she said.
TSB
For more news about the novel coronavirus click here.
What you need to know about Coronavirus.
For more information on COVID-19, call the DOH Hotline: (02) 86517800 local 1149/1150.
The Inquirer Foundation supports our healthcare frontliners and is still accepting cash donations to be deposited at Banco de Oro (BDO) current account #007960018860 or donate through PayMaya using this link.